A Mother’s Fight Against Cervical Cancer
A mother of three who ignored irregular periods and heavy bleeding for over a decade has shared her harrowing story after nearly losing her life to cervical cancer at the age of 43. Her experience serves as a powerful warning to other women to not ignore their bodies and to prioritize regular health check-ups.
Pamela Alexander, now 56, is a support assistant from Greenock, Scotland. She had her first smear test at the age of 22, and the results were normal. However, a panic attack during the procedure left her terrified of medical professionals. “I was embarrassed and scared of doctors,” she said. “After that, I never went back, even when I had my three children and received NHS reminder letters.”
Over the years, she began experiencing heavy bleeding, clots, back pain, and discomfort during sex. Despite these symptoms, she chose to ignore them, focusing instead on work and childcare. It wasn’t until August 2012 that her body forced her to confront the truth. “The bleeding just wouldn’t stop,” she recalled. “It was like turning a tap on. I collapsed in my hallway, covered in blood, and my partner called an ambulance.”
At the hospital, doctors discovered a tumour “the size of a tennis ball.” Ms. Alexander was initially told she had stage 2B cervical cancer, which was later upgraded to 3B, meaning it had spread beyond the cervix. 

“The gynaecologist said there was nothing they could do,” she said. “The tumour had spread to my bladder, bowel, and lymph nodes. It was awful, and I felt guilty for what I’d put my family through.”
A private specialist later offered multiple types of treatment, and she began chemotherapy, radiotherapy, and brachytherapy, a type of internal radiation. She suffered severe side effects, including hair loss, fatigue, burning sensations, and numbness in her fingers and toes. “It was horrific,” she said. “Brachytherapy was worse than childbirth. Chemotherapy nearly sent me into anaphylactic shock, but the alternative worked.”
By April 2013, Ms. Alexander was in remission. “It was the best feeling ever,” she said. “Even after five years, I was convinced it might come back. Reaching that five-year mark was incredible.”
Today, 14 years after her diagnosis, Ms. Alexander is registered disabled due to treatment-related complications, including brittle bones that caused a severe spinal injury last year. She praised NHS England’s rollout of at-home HPV testing, saying it could have saved her life. “It’s amazing and will change lives,” she said.
Ms. Alexander now warns others: “Please don’t be silly like me. A five-minute smear test could save your life. Go to the doctor. Don’t wait.” “I have four beautiful grandchildren I never would have seen if I hadn’t survived,” she added.
Understanding Cervical Cancer
Cervical cancer affects the cervix—the opening to the womb—and is almost always caused by long-lasting infection with certain types of human papillomavirus (HPV), a common virus spread through sexual contact.
Worldwide, it is the fourth most common cancer in women. In the UK, around 3,000 women are diagnosed each year, with roughly 850 deaths, while in the US there are about 14,000 new cases and 4,000 deaths annually.
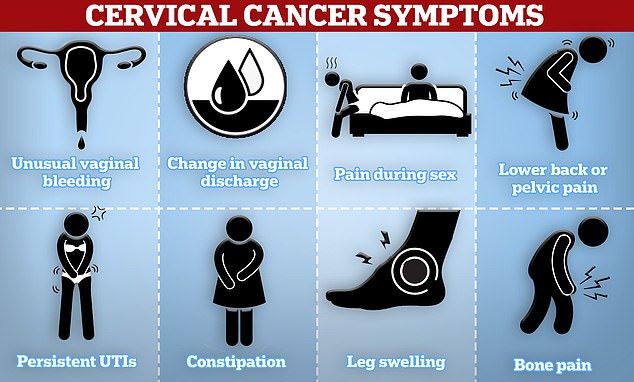
Warning signs can include unusual vaginal bleeding, pain during sex, pelvic pain, or unusual discharge, though early stages often cause no symptoms. Treatment depends on how advanced the cancer is and may include surgery, radiotherapy, or chemotherapy.
In the UK, women aged 25 to 64 are invited for cervical screening every five years, which now checks for high-risk HPV. In the US, screening usually begins at 21, using smear tests, HPV tests, or both.
The HPV vaccine has already led to huge drops in infections and early cell changes, with studies showing cervical cancer rates falling by up to 90 per cent in vaccinated women—making it one of the most preventable cancers if screening and vaccination are taken up.