Understanding Polycystic Ovary Syndrome (PCOS)
Polycystic ovary syndrome (PCOS) is a common hormonal disorder that affects many women worldwide. Despite its name, recent research suggests that women with PCOS do not have a higher rate of abnormal ovarian cysts compared to those without the condition. This finding has sparked discussions about the need for a name change to better reflect the true nature of the syndrome.
Key Findings from the Study
A study published in JAMA Internal Medicine analyzed data from 1,235 Finnish women and found that women with PCOS were 12 times more likely to have multiple antral follicles but did not have a higher rate of dominant follicles or abnormal, non-cancerous ovarian cysts. The research was led by Terhi Piltonen, a professor at the University of Oulu in Finland, who emphasized the importance of this population-based study in understanding the condition.
The researchers noted that their findings support a global movement to rename PCOS. They stated that the concern over pathological ovarian cysts in PCOS is unfounded. This aligns with the views of many women’s health specialists who believe the current name does not accurately represent the condition.
What Is PCOS?
PCOS is a lifelong condition that affects several organs and can lead to infertility, type 2 diabetes, and other metabolic issues. The exact cause is not fully understood, but there may be genetic or environmental factors involved. Diagnosis typically requires two out of three symptoms:
- Irregular menstrual periods or abnormal ovulation
- Increased facial or body hair, acne, weight gain, and hair loss due to higher levels of androgen
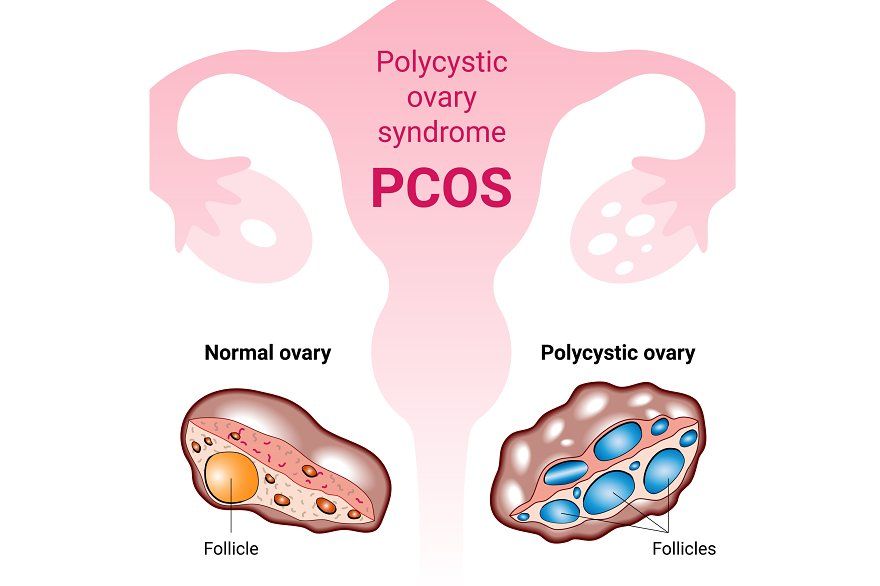
- The presence of 20 or more small fluid-filled sacs on an ultrasound, known as “antral” follicles
Many women with PCOS experience insulin resistance, which increases the risk of long-term health problems such as type 2 diabetes, high blood pressure, cardiovascular disease, and obesity.
Challenges in Diagnosis
It can take up to 10 years to diagnose PCOS, leading to missed opportunities for early intervention. Devini Ameratunga, a reproductive endocrinologist in Brisbane, highlighted the issue of both under-diagnosis and over-diagnosis, as not all women with PCOS present in the same way.
Not All Follicles Are Cysts
The JAMA study used data from the Finnish Women’s Health Study (WENDY). Researchers compared ultrasounds of 1,012 women diagnosed with PCOS to 223 women without the condition. They found that while women with PCOS had more antral follicles, they did not have a higher rate of abnormal cysts.
Dr. Ameratunga explained that the name PCOS was inspired by antral follicles, which can sometimes resemble cysts. However, these follicles are different from cysts and do not require the same level of medical attention.
Implications for Medical Practice
The study suggests that women with PCOS do not need more frequent ultrasounds to detect benign or pathological non-cancerous ovarian cysts. Magdalena Simonis, a GP and women’s health expert from the University of Melbourne, described the study as “really important” and noted that measuring ovarian cyst numbers does not correlate with the condition’s cardio-metabolic effects.
Limitations and Future Research
While the study provides valuable insights, it has some limitations. For instance, 97% of participants were white Europeans, and ultrasounds were performed on random cycle days by five different clinicians. These factors could affect the generalizability of the findings.
Global Push for a Name Change
Researchers behind the JAMA study argue that the findings support a global effort to rename PCOS. Professor Piltonen described the current name as “confusing” and said it has led to the syndrome being viewed as an ovarian disease. She emphasized that the ovaries in women with PCOS are “full and lush” with small under-developed follicles rather than large cysts.
Dr. Simonis and Dr. Ameratunga agree that the current name does not accurately reflect the condition’s broader health impacts. A name change, they suggest, would shift the focus away from the presence of ovarian cysts and highlight the metabolic and psychological aspects of the syndrome.