Rising Concerns Over NHS GP Services
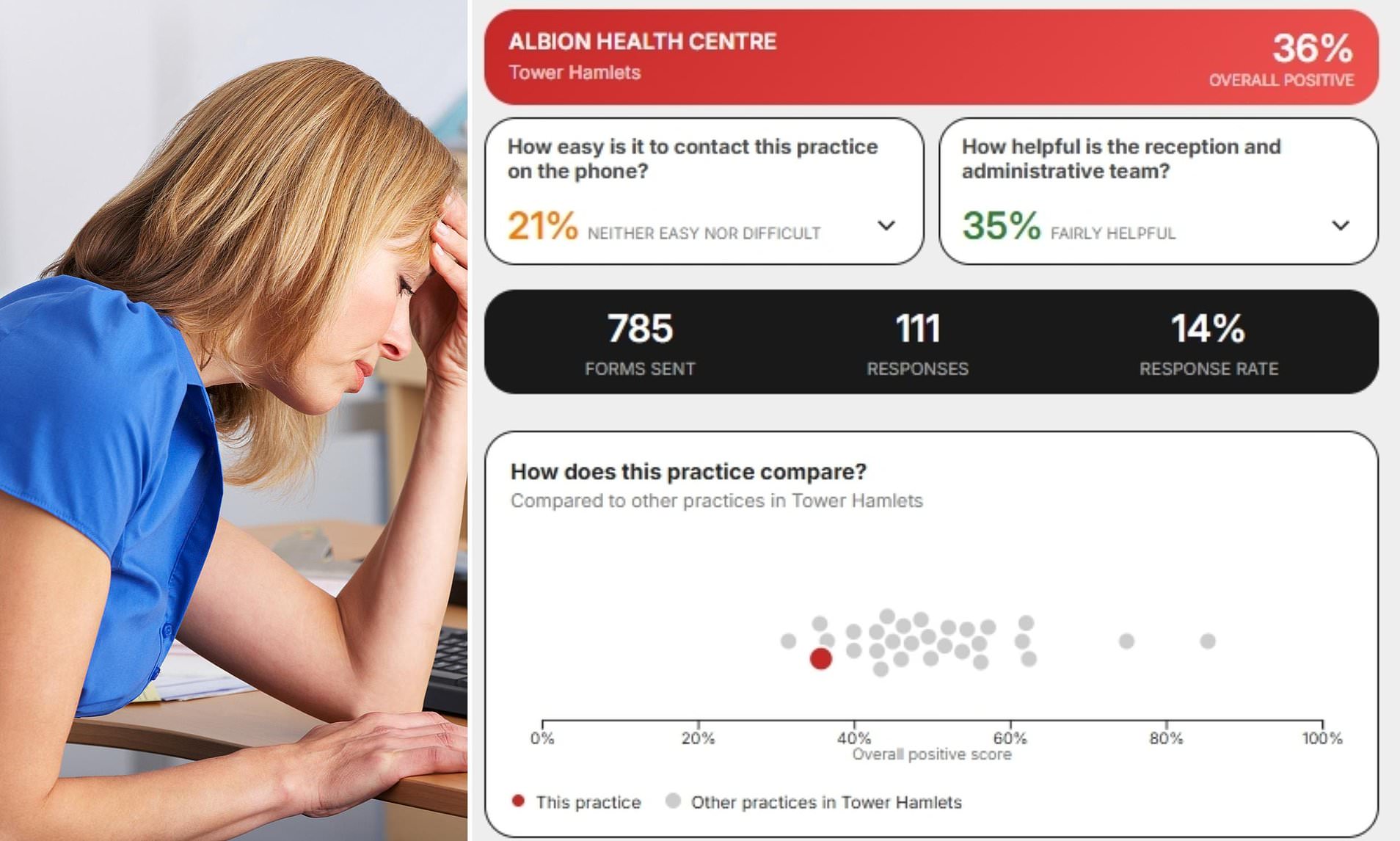
The quality of care provided by General Practitioners (GPs) within the National Health Service (NHS) is facing increasing scrutiny. Recent data indicates that over 134,000 written complaints were made about GPs in the past year. These complaints often revolve around communication issues, a lack of compassion, and staff attitudes, highlighting a growing dissatisfaction among patients.
The data from NHS Digital reveals that a significant number of patients are unhappy with their experiences, feeling that the system is difficult to navigate and potentially putting them at risk of serious health complications. Common issues raised include medication errors, impaired decision-making, and treatment delays. Around one in ten patients reported reduced attention and rude or disrespectful behavior from staff, with experts suggesting that workload is contributing to unacceptable errors in judgment.
Challenges in Accessing GP Services
A recent survey suggests that almost half of the public now avoid or delay contacting their GP due to falling numbers of family doctors and worsening standards of care. This trend is particularly concerning for elderly patients, who are being forced to book appointments online against NHS rules that require a range of booking methods.
Since 2017, nearly a quarter of GPs have left the NHS. In June last year, there were only 28,000 fully qualified full-time equivalent GPs, which is 1,000 fewer than in June 2017. This has resulted in only one GP per 2,200 patients, an increase of 70 patients per doctor since 2020. The situation is even more dire in deprived areas where demand is highest, creating a stark postcode lottery.

Impact on Elderly Patients
Re-engage, a charity focused on tackling loneliness in old age, warns that it is becoming increasingly difficult for elderly people to see a GP. Despite NHS contracts requiring all practices to allow patients to book appointments over the phone or in person, a third of patients over the age of 75 are being forced to use online forms if they want to see a doctor. Some patients reported being forced to choose between online forms and talking to an AI chatbot over the phone, both of which they found difficult to navigate alone.
This situation leaves vulnerable people forced to self-medicate, turn to overcrowded Accident and Emergency departments, or simply hope that their symptoms will resolve on their own. Critics are calling for surgeries to be penalized if they are found to be flouting contract requirements that protect equality.
Calls for Improved Access
The report, Care on Hold, asked 926 older people about their recent experiences of accessing GP services. It found that the loss of GPs and face-to-face appointments has led to an increase in feelings of inadequacy and rejection among patients. Jenny Willott, chief executive of Re-engage, stated that many older people are being pushed toward digital routes they cannot easily use. She emphasized that while digital tools and AI can play a role, they cannot replace human contact, which is often a vital lifeline for older people who are lonely or socially isolated.
Government Initiatives and Challenges
In response to these challenges, the government has promised to boost access to family doctors in England through a new GP contract backed by a £485 million investment. Since October, GPs have been required to keep online booking systems open all day from 8am to 6.30pm. This change was intended to improve access and end the 8am telephone battle for appointments. However, critics argue that this has added to the NHS workload, pushing up waiting times and reducing appointment length times to make time for triaging.
Some surgeries have extended staff hours, meaning some are being paid just 30p a day for every patient registered with them. Others are using AI to triage requests and free up staff time. In some instances, this has led to a breakdown in communication, with patients left unsure of what the next steps are or even how to book an appointment.
Personal Experiences
Maureen, 88, is one of the hundreds of elderly patients left in limbo despite suffering from a suspected thyroid problem. She described the process of getting a doctor’s appointment as a nightmare, with long waits and unclear next steps. “Trying to get a doctor’s appointment is a nightmare. You have to call at 8am and after hanging on you are eventually told all the appointments have gone and to call back the next day. It’s like an endless road.”
NHS Response
In response, an NHS spokesperson told the Daily Mail: “While online booking forms offer patients an additional way to access care, they are not a replacement for traditional methods, and all GP practices are contractually required to allow patients to book appointments by phone or by attending reception in person. We have upgraded thousands of GP telephone systems, and by expanding the hours for submitting initial online requests we are freeing up phone lines for those who prefer to make an appointment by phone.”
Future Outlook
In February this year, the government promised to improve access to family doctors in England through a new contract mandating all patients with urgent needs to have access to a same-day appointment. However, Professor Victoria Tzortziou Brown, Chair of the Royal College of GPs, believes the pressure GPs face as ‘the front door of the health service’ is unsustainable. She expressed concern that some patients are delaying or avoiding seeking care because they think getting an appointment will be difficult. GPs are working harder than ever, but she acknowledges that too many patients are still waiting too long for appointments or are anxious that they won’t be able to get the care they need when they need it. “GPs and our teams are just as frustrated as our patients when they can’t access our care.”